APHASIABANK GRAND ROUNDS
Audrey L. Holland
Davida Fromm
Margie Forbes
Brian MacWhinney
These materials are provided to students and clinicians who wish to improve their understanding of aphasia. None of these materials should be copied or used anywhere outside of these web pages. In particular, none of the videos should be download or copied and placed anywhere else. Users should adhere to the Ground Rules for use of TalkBank data.
INTRODUCTION
Davida Fromm
Margie Forbes
Brian MacWhinney
These materials are provided to students and clinicians who wish to improve their understanding of aphasia. None of these materials should be copied or used anywhere outside of these web pages. In particular, none of the videos should be download or copied and placed anywhere else. Users should adhere to the Ground Rules for use of TalkBank data.
INTRODUCTION
Margie Forbes
Brian MacWhinney
These materials are provided to students and clinicians who wish to improve their understanding of aphasia. None of these materials should be copied or used anywhere outside of these web pages. In particular, none of the videos should be download or copied and placed anywhere else. Users should adhere to the Ground Rules for use of TalkBank data.
INTRODUCTION
Brian MacWhinney
These materials are provided to students and clinicians who wish to improve their understanding of aphasia. None of these materials should be copied or used anywhere outside of these web pages. In particular, none of the videos should be download or copied and placed anywhere else. Users should adhere to the Ground Rules for use of TalkBank data.
INTRODUCTION
These materials are provided to students and clinicians who wish to improve their understanding of aphasia. None of these materials should be copied or used anywhere outside of these web pages. In particular, none of the videos should be download or copied and placed anywhere else. Users should adhere to the Ground Rules for use of TalkBank data.
INTRODUCTION
The primary goal of this resource is to introduce, illustrate, and discuss the different types of aphasia one encounters in clinical practice. In assessing these types, you will want to take into account formal test results and also your general knowledge and information about what you see and hear, which may differ from test results. The aphasia types we use here are from the Western Aphasia Battery (WAB), which is the formal aphasia assessment tool used in the AphasiaBank project. While there are other classification systems, this one is used by many aphasiologists in the United States and elsewhere. The WAB aphasia type gives a sense of the pattern of language performance, and the WAB Aphasia Quotient (AQ) indicates the severity of the aphasia. However, our video samples are not from WAB testing, but from the AphasiaBank protocol tasks, so we focus on discourse.
It is important to know how language use differs among these aphasia types, first because they provide some information about the localization of language functions in the brain, and more importantly for our purposes, because they help to inform a plan for therapy. This is true both for therapy addressing the impairment itself (“impairment-focused” treatment) and for treatments directed at improving everyday communication and functioning (“consequences-focused” treatment).
This leads to the secondary goal of this resource, which is to raise relevant questions about treatment of some of the communication problems we see in aphasia. Most of the questions posed here have no right or wrong answers. They are intended to stimulate discussion about approaches to clinical intervention.
While we will concentrate on the many ways that language differs among individuals with aphasia, you will note commonalities as well. Word-finding problems are probably the most notable, but there are others. For example, “little” words, such as pronouns and articles, are almost always problemmatical, and simpler grammatical constructions are more likely to be correctly used than complex ones. For many of the people presented here, gender terms (e.g., sister, brother, man, woman, he, she) present special challenges. For short video examples of word finding problems, agrammatism, and other typical features of aphasia in connected speech, see Examples. Finally, although comprehension of spoken language is quite good in some individuals with aphasia, even those with mild Anomic aphasia sometimes get tripped up by the language of communication partners, movies, or TV programs. Below are some suggestions for helping you become an effective communicator with people who have aphasia:
- Speak a bit more slowly than you might speak to a good friend, but be careful to preserve your natural prosody.
- Keep your sentences on the simple side, if you can.
- Try to keep noise and distractions to a minimum.
- You might want to talk a little bit more loudly, since many people with aphasia are older.
- Learn to use and follow the principles of Supported Communication (Kagan,1998) in your interactions with aphasic individuals, outside the restrictions imposed by formal aphasia tests.
- Above all, check with the aphasic person about what you might do to facilitate good communication with him or her.
One more thing before we get down to work. We have chosen here to call our aphasic “stars” by their first names. (Well, not REALLY their first names -- in all cases, we have used pseudonyms, in line with our human subjects regulations). Generally, we do not advocate calling clients by their first names. Rather, we believe we should respectfully ASK people what their name preferences are, and follow their choice. We have done that in all of these cases.
POSTERIOR VS ANTERIOR DAMAGE
When you first meet a person with aphasia, note whether he or she is paralyzed or weak (hemiplegia or hemiparesis) in the arm and leg on one side of the body (most frequently, the right side). This provides a clue about whether the aphasia is a fluent or a non-fluent one. Because a posterior brain lesion interferes only minimally with either the white matter tracts that connect to the brain’s anterior motor structures for speaking and movement or to those anterior motor structures themselves, it tends to result in a fluent aphasia. Anterior lesions, on the other hand, frequently damage these motor areas, usually resulting in nonfluent aphasia, along with arm and/or leg paralysis or paresis. The exception, of course is global aphasia, where BOTH posterior and anterior brain structures are affected.
We will start by distinguishing a fluent aphasia, Wernicke, from a nonfluent aphasia, Broca. This is the clearest of the examples.
WERNICKE APHASIA
Description
People with Wernicke aphasia typically speak easily and with near-normal prosody, even though their output is often unintelligible. Their speech frequently contains errors such as wrong words (semantic paraphasias), made-up words (neologisms), or even extended jargon (strings of incomprehensible output). The more severe the aphasia, the more problems of this sort they demonstrate. People with Wernicke aphasia have difficulty understanding spoken language, including their own, with one result being that they cannot effectively monitor their own productions. They have similar problems with reading and writing, although occasionally one finds an individual with Wernicke aphasia with disproportionately preserved ability to read and sometimes, in mild cases, to write. For them, these relatively well preserved abilities become “nuggets of gold” that can be used to help them understand what they hear.Example #1
The first example of Wernicke aphasia is Barry, who is severely impaired. Barry was a Corrections Officer, but he retired after his stroke. His Aphasia Quotient (AQ) on the Western Aphasia Battery (WAB) was 28.2 when he was tested in 2009, 5 years after his stroke. His WAB Auditory Comprehension subtest scores were 58/60 for Yes/No Questions, 32/60 for Auditory Word Recognition, and 18/80 for Sequential commands, yielding a composite Auditory Verbal Comprehension score of 5.4/10. The language sample below is from that 2009 session. It should be noted that he was retested in 2014, and he had improved! The new WAB AQ was 37.8, although he still had severe Wernicke aphasia.
Listen to a few minutes of his speech and then consider the discussion questions that follow. Margie, his interviewer, is asking about his stroke and its consequences, and about a meaningful experience in his life.Questions for discussion
How would you describe what you heard?
Margie asks him how his speech has changed? He replies, “A little bit bigger.” What does he mean? What do you think of her interpretation?
She asks, “What did you do to get better?” He answers, “Walking”, then repeats “Walking” while gesturing toward his throat and mouth. Does he mean “walking”?
Note that he said “walking” and his gesture used both hands. Do you get a clue that his aphasia is fluent from the fact that he does not appear to have a hemiplegia?
Barry notes, “Some I get. Some I can’t. And I just have to pend what I have and have to get.” How do you interpret this? Do you think it is an accurate appraisal?
Barry then tells his “Important Event” story. It is basically about his military service. How much of it do you understand? What branch of the service was he in? Was he trained as a pilot? What do you think he meant by “my shooed was ressle”? Even though most of these substantive “words” are nonwords, they don’t break the rules of English phonology. What do you make of this ?
Do you agree with our conclusion that Barry is severely aphasic? That he has fluent aphasic speech? Are you prepared to guess where his lesion is?
Example #2
The second sample of Wernicke aphasia is Chuck. He is 60 years old and has an AQ of 36.8. Chuck is a college graduate and worked in the computer industry until the onset of his stroke, which resulted from a ruptured arterio-venous malformation (AVM). His Auditory Verbal Comprehension composite score was 5/10, with these raw scores on the three subtests: 57/60 on Yes/No Questions, 37/60 on Auditory Word Recognition, and 6/80 on Sequential Commands. He talks first about his problems (speech video), then tells a familiar story (Cinderella video), and then does a bit of the Boston Naming Test (BNT, short form -- naming video). Watch his gestures carefully.
Questions for discussion
Chuck tries to explain to Margie what his problem is. How well does he communicate it?
You all know the story he is telling in the second segment. But do you you recognize it? What story is it? What gave you the clues?
Did you notice his gesture as he was trying to name “cactus”? What did he do? In the southwestern U.S., a cactus like the one pictured in the BNT is more likely to be called “saguaro”. Would this be a right or a wrong answer? Is it important for you to be aware of regionalisms such as this?
Chuck is a very good example of someone who speaks “extended English jargon”. Other than the onomatopoeic sounds that he occasionally makes (we suspect to the delight of his listener), he mostly uses real English words. Yet we cannot understand much of what he is saying. How does this compare with Barry’ speaking patterns?
What are Chuck’s strengths? Please do not limit yourself to language!
Treatment focus -- Barry and Chuck
For planning Barry’s treatment, it is a good idea to look at both his strengths and his weaknesses in relation to language (impairment), and also his general communicative ability (effects of his impairment on his communication).
Please note these strengths:
- He understood some of the questions, but not all of them.
- What did Margie do to facilitate his comprehension?
- What else could she have done if Barry had been her patient and this had been a therapy session?
- Did he give her clues that helped her to help him understand? Would it be worthwhile to teach others to use this strategy?
- He demonstrates appropriate conversational style.
- Would you try to modify his style? Why or why not?
- He uses a mixture of real words, neologisms, and jargon.
- Would you attempt to modify his neologisms and jargon? If so, how? Why?
Some clinicians might choose to work on things that the individual CAN’T do. What are some of Barry's "weaknesses" that you might consider addressing in treatment? For direct work on his impairment, would you be more interested in improving his comprehension or decreasing his jargon? Why? How?
We have no information on Barry’s reading aloud or his silent reading comprehension. If he were reading relatively well, how might you include it in treatment aimed at reducing his neologisms, semantic errors, and his jargon?
If his reading corresponded in severity to his speech output, would you attempt to improve it? Why? Would there be any value in focusing treatment on reading common signs, such as “stop”, “no exit”, etc.
We would like to meet a clinician who is not challenged by Chuck. We certainly are. As with Barry, we have no information on reading or writing. If he could read single words, do you think that could be utilized in treatment? How?
How can Chuck’s non-linguistic strengths be mobilized in the treatment of his aphasia?
How well do you think that either of these two men might do with Visual Action Therapy (VAT) by Helm-Estabrooks? Would they likely respond differently or similarly?
Paraphasias -- semantic
The following video clips provide some good examples of the types of semantic paraphasias -- substitutions of one word for another -- seen in individuals with Wernicke aphasia and other aphasia types as well. Often the substituted word is related in meaning to the target word (e.g., “foot” for “shoe”, “raincoat” for “umbrella”, “king” for “prince”, “sailor” for “fireman”, “dog” for “cat”). The first two examples are from a man with Wernicke aphasia; the final example is from a woman with Anomic aphasia. All of these examples are from their Cinderella stories.
Can you transcribe the paraphasia in each case?
BROCA APHASIA
Description
In contrast to those with Wernicke aphasia, people with Broca aphasia speak with many hesitations, pauses, and short phrases. Their speech includes phonemic paraphasias (substitution, addition, omission, or rearrangement of speech sounds in words), disturbed grammar (agrammatism), and slow and labored speech. Often, they also have apraxia of speech (disruption in motor speech programming) and dysarthria (disturbances in muscular control -- weakness, slowness, or incoordination -- of the speech mechanism). (And yes, it is often difficult to differentiate which is which!) However, in many cases, people with Broca aphasia can get their messages across. They tend to use more nouns than verbs in spontaneous speech, and they often have trouble with functor words (e.g., pronouns, articles, prepositions) both when speaking (production) and when listening to others (comprehension). Language comprehension and reading are typically less impaired than speech. Complex sentence structure is often compromised in both comprehension and reading. This is called “asyntactic comprehension”.
Example #3
Gloria’s speech pattern is consistent with Broca aphasia, and her WAB AQ is 40.9. Her speech is extremely agrammatic. Before her stroke, caused by the rupture of an aneurysm in her brain in 2006, she ran a personalized cake baking and decorating service. Gloria tells the Cinderella story in the sample you will hear. Note the limited movement in her right arm and hand.
Questions for discussion
How would you describe what you heard?
Did you notice anything to suggest that Gloria has concomitant apraxia of speech? Dysarthria?
Did you notice the quality of her facial expressions and her gestural language? What do you make of it?
How about her description of the fairy godmother?
One of the devices she uses in her communication is word repetition, such as “dancing, dancing, dancing”. Why do you think she does that?
Did you notice short runs of fluency in her speech? Can you remember one? (This is not uncommon in people with Broca symptomatology.)
Did you also notice that she provided a little summary of her story at the end?
Why do you think she sang “Wish upon a star”? Is it correctly a part of the Cinderella story? Is including a song from a different Disney movie a kind of semantic paraphasia? Did you notice the phonemic paraphasias for both "wish" and "star" the second time she sang the song (at the end of the clip)? This is a lovely illustration of the variability common in aphasia.
Does Gloria show a disproportionate difficulty with verbs as opposed to nouns?
Gloria did not return to her baking service. Do you think her speech or her hemiplegia is the greatest deterrent to her returning to her occupation?
Treatment focus - Gloria
A number of well-researched treatment approaches seem to work best with individuals who have Broca aphasia. Among them are: Treatment of Underlying Forms (TUF) by Thompson and colleagues; Verb-strengthening Network Training (VNeST) by Edmonds; Scripting by Youmans, Holland, Cherney, and others; and Visually Assisted Speech Technology (VAST) by Williamson. Would you consider using any of these approaches with Gloria? Why or why not? Consider which of these techniques are designed to deal with everyday communication or with overcoming Gloria’s difficulties, or both. Does that matter?
Gloria’s strengths appear to include organizing a narrative task, good and informative gestures and repetition, the ability to express emotions by meaningful voicing, and repetition. How might you use these in your work with her?
Do you believe it might be helpful to incorporate some apps into Gloria’s treatment? Which apps? Why?
Example #4
Patrick is almost 81 years old, 12 years post-stroke and severely impaired, with an AQ of 17. Given his limited speech, he may initially appear to be globally aphasic. Yet his auditory comprehension scores on the WAB are well above the cutoff for Global aphasia. He has very severe Broca aphasia with apraxia of speech, according to his clinician’s assessment. His limited output in these examples does not give you much of an opportunity to judge his speech behaviors. However, as you will be able to see, despite limited verbal expressive skills, he is clearly able to understand the task (telling how to make a peanut butter and jelly sandwich) and to communicate rather successfully using the photo stimuli and gestures.
Patrick’s motor speech difficulties likely contribute disproportionately to his paucity of speech. In this next sample, you can further observe his inventiveness in communicating, another characteristic not often seen in Global aphasia. The video segment is from another inventory being developed by AphasiaBank, Famous People Protocol (FPP), specifically designed to permit people with severe aphasia, such as severe Broca aphasia, apraxia of speech, and Global aphasia, to utilize their best strategies as they identify pictures of famous people. Watch this brief example of Patrick doing this task, specifically the stimuli for Marilyn Monroe, Jay Leno, Elizabeth Taylor, and Elvis Presley.
Questions for discussion
Do you have any sense of this man’s personality? What do you think it would be like to work with him? If you were in a setting where this was possible, what do you think it would be like to have him in an aphasia group?
Example #5
Ralph’s sample is also is from the FPP, specifically the stimuli for John Wayne, Michael Jackson, Judy Garland, and The Beatles. Like Patrick, Ralph has severe Broca aphasia and says only a few simple words, but because he scored better than Patrick on the WAB Auditory Comprehension subtests, his 28.7 AQ is higher than Patrick’s. He was 5 years post-stroke when this video was made. The clinician is encouraging him to communicate as best he can in any way possible.
Questions for discussion
What can you detect about Ralph as a person from his communication with the clinician?
Please note Audrey’s error, and what she does about it. Did she handle it well? Did Ralph handle it well? What do you think about clinicians making mistakes? Is this necessarily a bad thing? Why or why not?
Treatment focus -- Patrick and Ralph
Does the amount of time since their strokes influence how you might want to structure their therapy? Why and how?
Do any of the suggestions raised for Gloria’s treatment make similar sense for Patrick or Ralph? Why or why not?
Both of these speakers have good gestural potential. If you should decide to work on gestures, what would you do? Would you consider Visual Action Therapy?
Why would it be important to know something about their reading and writing abilities?
For Patrick, it’s possible that the severity of his motor speech problems may outweigh his expressive language problems. What kinds of things might you do to investigate that further? Assuming you confirmed the presence of severe AOS, how would that influence what you might want to do with him in treatment? Of the various approaches reported in the literature (by Helm-Estabrooks, Rosenbek, Youmans, Williamson, Wambaugh, Duffy, and others), which, if any, would you consider undertaking given the long time post-onset. Why?
It should be noted that Audrey’s and Margie’s style in these videos differ markedly. This reflects the difference in the measures they are using. Margie is administering the AphasiaBank Protocol, whereas Audrey is administering the Famous People Protocol. The primary goal of AphasiaBank is to deliver a large uniform sample of spoken language from aphasic people, collected in a systematic and reliable manner, without cuing from the examiner, for aphasia researchers and educators to use in their work. However, a significant segment of the aphasic population is unable to participate in this protocol, because their aphasia is too severe for them to produce language samples.
The Famous People Protocol is specifically designed to tap into the communicative competencies of people with severe aphasias, and requires the tester to find ways to seek COMMUNICATIVE as opposed to LINGUISTIC abilities. Thus, various avenues of communication beyond language are explored in a systematic manner with the goal of finding out what a person actually KNOWS and how he or she can best communicate it. This requires a different set of clinical skills from the ones required to systematically gather explicit linguistic data. Our best guess is that clinicians should have both sets of skills, and that the former is most important for diagnosis, the latter most critical for treatment.
Paraphasias -- phonemic
Following are some examples of phonemic paraphasias -- one or a few incorrect sound(s) in the target word. These paraphasias are often seen in Broca speakers, but like semantic paraphasias, occur frequently in other types of aphasia as well. In fact, paraphasias are a general feature of aphasia. The following examples of phonemic paraphasias are from speakers with Broca aphasia. These segments are taken from descriptions of the “Window” picture sequence (shown below), the “Umbrella” picture stimulus (shown below), the Cinderella story, and a stroke story.
Window
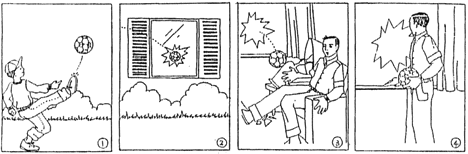
Umbrella
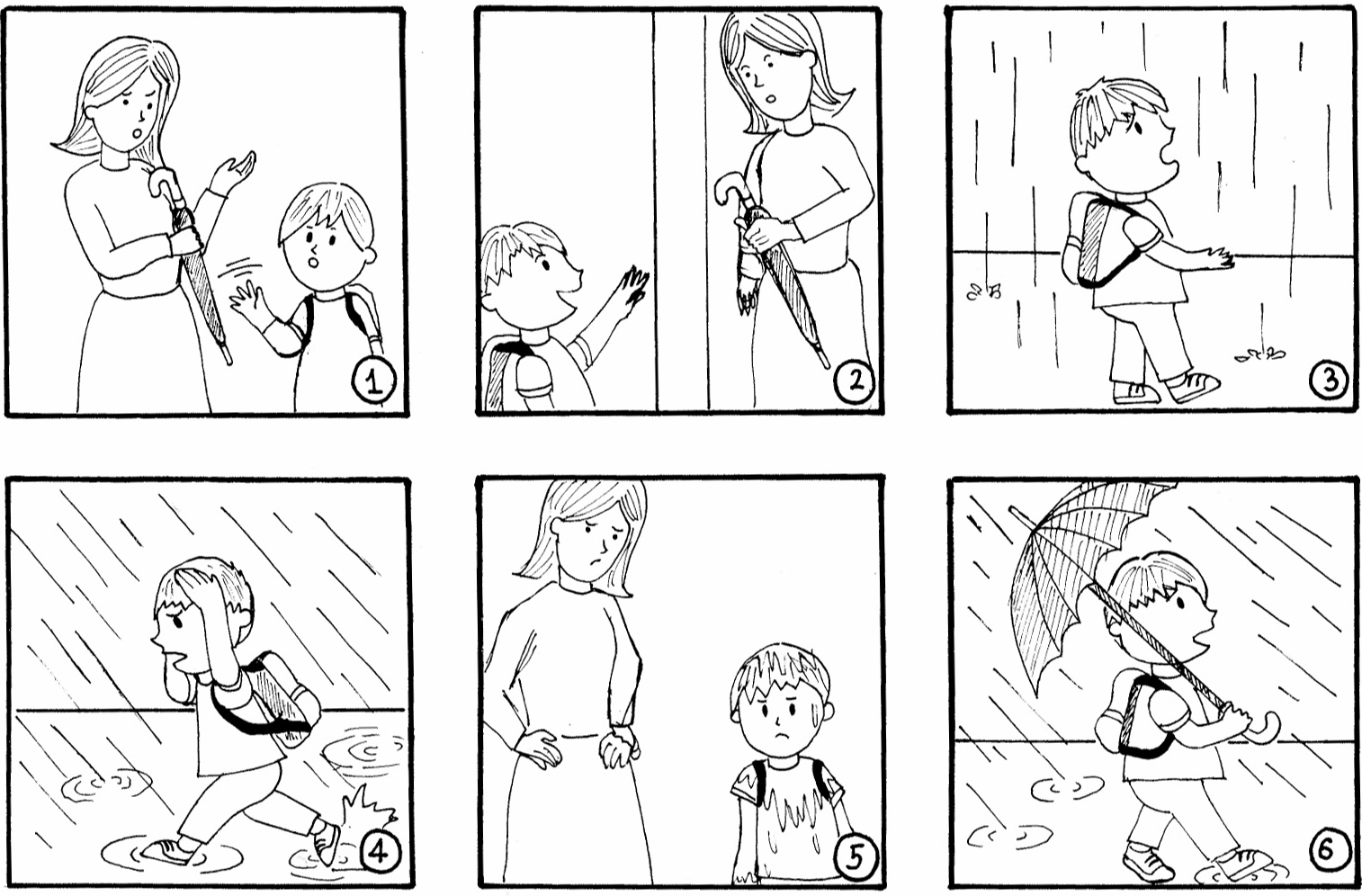
For each of these, what is the target word? Can you transcribe the error phonetically or not?
GLOBAL APHASIA
Description
Severe communication limitations, including difficulties with comprehension and production, are typical of people with Global aphasia. AOS and/or dysarthria may be present as well. Reading and writing are usually impaired, although if a global patient has even modestly preserved reading and writing skills, these are strengths to capitalize on in treatment. Given the nature of the vasculature that produces these global language problems, it is also highly likely that their strokes will be accompanied by hemiplegia.
Examples #6 and #7
The two people you will be watching are Bill and George. Their output resembles that of Patrick and Raph. However, they also have significant difficulty understanding what is being said to them, so their auditory comprehension is similar to that of Barry, our Wernicke example. Bill and George are shown participating in the FPP. Bill is looking at stimuli for Judy Garland, The Beatles, and Marilyn Monroe; George is looking at The Beatles, Marilyn Monroe, and Elvis Presley. Look for differences in their ability to communicate, despite their global language problems.
Questions for discussion
Who is the better communicator, Bill or George? What do you think accounts for the difference?
They both have limited comprehension as well as obvious speaking difficulties, but they clearly have some linguistic differences. Which one do you think has the better resources for communicating?
Treatment focus -- Bill and George
Let us suppose that they are both newly aphasic, about 3 months post-onset. Would you approach their treatments similarly? Why or why not?
What would be a most valuable first step for Bill? Why? What are some approaches with strong evidence support that you might try? Would you include motor speech work?
It is important to look for strengths in all aphasic individuals. Indeed some clinicians center their treatment on the aphasic person’s relative linguistic strengths, as well as the non-linguistic strengths they bring to their treatment. If you take a strengths-based approach with George, what might you want to work on? What personal characteristics seem to be strengths?
ANOMIC APHASIA
Description
Anomic aphasia is another fluent aphasia, but it is quite different from Wernicke aphasia. The hallmark of Anomic aphasia is word-finding problems, which disrupt the easy flow of speech. People with Anomic aphasia generally have relatively high WAB scores and less severe overall language impairments. Their auditory comprehension is usually only mildly impaired if at all. However, the following samples will clearly demonstrate serious word-finding difficulties as well as compensatory strategies for dealing with them. You will again hear paraphasias and see lots of signs that these speakers are struggling for words.
Example #8
Sandra, in her early 40's, has a very high WAB score of 92.8. She is an architect, but has not been able to work since her stroke. She has two small children and a devoted spouse.
Questions for discussion
Did you notice Sandra's runs of fluency as well as her long pause patterns?
Did you notice how the word “godmother” came to her a little while after she had given up on finding it? What explains that?
Did you notice how Sandra cued herself to explain about the mice turning into horses? Is this perhaps a form of circumlocution, or “talking around” the intended word or idea?
What did you think of her sentence structure and story-telling?
If you had to come up with a one-word description of Sandra's speaking style, what would it be? Why did you choose this word?
Do you think Sandra may have other problems besides aphasia that are suggested by her speech?
Example #9
Here is another Cinderella clip that further illustrates some characteristics of Anomia. Violet scored 89.5 on the WAB AQ. She is in her early 60's and has had some advanced education. She was employed as a bookkeeping specialist before her stroke resulted in her retirement.
Questions for discussion
Did you notice that Violet had both kinds of paraphasias (semantic and phonemic) and circumlocutions, as in “the lady who comes and gives the wishes”?
Did you notice a strategy she used when she couldn’t think of a specific word like “Cinderella”?
What do you think of Violet’s self-monitoring?
Example #10
There are exceptions to the mildness of most Anomic aphasias. Greg is an example of that. Despite a right hemisphere stroke secondary to an AVM repair at the age of 23, he completed several graduate degrees and had a successful career, ending up as a senior executive for an IT company. At the age of 54, he had a left hemisphere stroke and was initially diagnosed as having a moderately severe Wernicke aphasia. When we saw him 2 years post-onset (from the left hemisphere stroke), his WAB AQ was 78.5 and his WAB classification was Anomic, with most of his language difficulties in production as opposed to comprehension. Here is his rendition of the Cinderella story.
Questions for discussion
Did you notice the frequent use of general terms instead of specific words? What other signs of word finding problems did you notice in his sample?
Did Greg use any compensatory strategies when he had trouble finding words and finishing sentences?
Greg’s aphasia type appears to have changed from Wernicke aphasia to Anomic aphasia. If improvement from Wernicke aphasia occurs, is this the most likely outcome?
How much of the Cinderella story could you retell from the information Greg provided?
Treatment focus -- Sandra, Violet, and Greg
A very well-studied and frequently-used approach to Anomic aphasia is to practice word-retrieval in a hierarchical order, beginning with recognizing, repeating and then naming words in increasingly complex tasks (such as reading), followed perhaps by finishing sentences using the words, naming other associated words, and finally creating sentences using the words that are the focus of treatment. (This is a simplification of many such hierarchical word practice tasks, but you get the general idea.) How useful do you think that would be for any of the three Anomic aphasic patients shown here? Can you explain why you say that?
Can you think of any reasons why discourse-level tasks as opposed to contextual word-retrieval tasks would be helpful to any of these people?
Do you think that adapting any of the techniques used in second-language vocabulary acquisition might be of value to either Sandra or Violet? Why? What about Greg?
Would it be worthwhile to inform your aphasic patients about the similarities between these “word-finding” problems and those that are associated with normal language use, particularly in aging?
Can you think of any apps that might be useful to persons with problems such as these?
CONDUCTION APHASIA
Description
A primary diagnostic characteristic of Conduction aphasia is that repetition skills are disproportionately worse than what you would expect from the person’s free speech skills. So, it is important here to show samples from a variety of tasks. One of the characteristics of Conduction aphasia is called conduite d’approche, where the person makes a series of incorrect approximations of the target word, sometimes, but not always, ending up with the right pronunciation of the word.
Example #11
This first set of 8 video clips comes from Jeff, a person we saw two times, 5.5 years apart. You’ll see him doing a variety of language tasks at the first visit, time “a”, and then you can hear how he sounds 5 years later at time “b”. Jeff had an AQ of 76.3 at the time of his first test and 81.1 at the second time. In both cases, his WAB subtest scores fit the pattern for Conduction aphasia.
Questions for discussion
Do you think Jeff changed from time a to time b in his free speech and Cinderella clips?
If you had not heard him repeating words in the repetition task, would you have called him Anomic?
Example #12
In these next 2 examples, you’ll hear Jerry tell a story about the “Window” picture stimulus and then do part of an AphasiaBank sentence repetition task. In his picture description, you’ll hear his repetitive effort (conduite d’approche) to produce the word “startling”. In the repetition task, he is repeating some sentences that have a simple core to which additional words or phrases are added. Jerry’s AQ was 76.3 and he was about 6.5 years post-stroke.
Window

Questions for discussion
Other than Jerry's repeated attempts to get the word "startling", did you notice any other unusual features of his speech?
Would his struggle for the word “startling” give you a clue as to his aphasia type? In the process of trying to say that word, did you notice other ways he tried to get the point across or cue himself?
What does it tell you about Jerry that he moved on with his story but then returned to the word that had given him trouble and produced it correctly?
Were you surprised by his poor repetition performance? Do you think it might be possible that the repetition problems shown by Jeff and Jerry are related to auditory-verbal short term memory problems instead of language problems?
Questions for discussion
Would you like to transcribe Helen’s speech? Why or why not?
Would you be surprised to know that Helen’s Auditory Comprehension subtest score on the WAB was 9.75 (out of 10)?
Does she seem to be aware of any of her errors?
Example #13
The next example is from Helen whose WAB AQ was 60.5. Her WAB repetition subtest score (2.5 out of a possible 10) was disproportionately lower than all of her other subtest scores. In this segment of the Cinderella story, she is telling about the glass slippers and the fairy godmother’s instruction to be back by midnight. An interesting feature of Conduction aphasia, in addition to the conduite d’approche and the frequency of paraphasic errors, is that when number words are interspersed with other nouns, they make speech disproportionately difficult. In Helen’s case, you can hear this in her difficulties with the “number-ish” word “midnight”. In general, much of her output is characterized by jargon. In fact, were it not for her scores on the WAB Auditory Comprehension subtests, she would have been classified as Wernicke's. She may simply have an unusual presentation, or this may be an example of where the psychometric properties of the formal test suggest a diagnosis that you as a clinician may question.
Questions for discussion
Would you like to transcribe Helen’s speech? Why or why not?
Would you be surprised to know that Helen’s Auditory Comprehension subtest score on the WAB was 9.75 (out of 10)?
Does she seem to be aware of any of her errors?
Treatment focus -- Jeff, Jerry, and Helen
A challenge for clinicians in working with people with Conduction aphasia is that most of us rely heavily on repetition, providing auditory models and using repetition tasks as a correction device in aphasia treatment. This avenue is closed for individuals with conduction aphasia, who are singularly unable to benefit from repetition. What are some ways you might get around this problem in your work with them? What could you use instead of auditory models?
Because most individuals with Conduction aphasia are well aware of their own speech errors (and attempts to correct them often turn into conduites d’approche), what would you advise your client to do when they occur?
You might wish to observe Jeff's short clips again. Remembering that his second sample in each case was made 5.5 years after the first one, do you believe that additional direct therapy is in order? Why or why not?
TRANSCORTICAL SENSORY APHASIA
Description
The Transcortical aphasias (Sensory and Motor) are less common than the other aphasia types. As with Conduction aphasia, repetition skills are key to the diagnosis of the Transcortical aphasias. However, in this case, the repetition skills are disproportionately better than what you’d expect from the free speech skills. So again, we will provide video examples of a variety of tasks from the same person so you can compare. In Transcortical Sensory aphasia, spontaneous speech is fluent and frequently contains paraphasias. Auditory comprehension is likely to be markedly impaired.
Example #14
Here is a series of 4 video clips from Millie, whose WAB AQ was 66.4. Millie was 63 years old, college educated, and almost 5 years post-onset of a hemorrhagic stroke secondary to a tumor. She continues to manage her home successfully.
Questions for discussion
If you met Millie at a noisy party, would you necessarily think she had aphasia? Why or why not? Do you think she gets along well in social situations with old friends?
If you didn’t know she was telling the Cinderella story, would you recognize it as such? Would you consider it a good story? What about her use of the word “beautiful”?
In her PB&J sandwich sample, can you explain why it ended up as a “ham sandwich”?
TRANSCORTICAL MOTOR APHASIA
Description
Again, with a Transcortical aphasia, repetition is disproportionately better than free speech and paraphasic errors are common. But, in contrast to Transcortical Sensory aphasia, the output in this case resembles the more nonfluent aphasia types and auditory comprehension may be somewhat less impaired.
Example #15
Donna is in her early 50’s and has had 14 years of schooling. Her slight hemiparesis has precluded her from continuing her work as a massage therapist, but she still manages to provide exercise sessions for other people in her aphasia center. Donna scored a 74.6 on the WAB AQ . These clips allow you to compare her word naming and word repetition to her free speech.
Questions for discussion
Donna’s speech is a treasure trove of phonemic paraphasias. You might want to listen again to any of the video clips and list the paraphasias that you hear. But it is important that you also be aware that she EXPECTS her listeners to take responsibility to interpret some of them correctly. An excellent example is the word “susceptible”, which is never even close to correct, but she is putting the burden on you to get it. Does that tell you something about her?
Her speech suggests that apraxia of speech coexists with her aphasia. How could you rule in or rule out coexisting dysarthria? Why does or doesn’t it matter?
How did you feel when she completed the repetition task successfully?
Given this brief sample, do you have any ideas about Donna’s resilience and adaptive capabilities?
Treatment focus -- Millie and Donna
For both of these relatively rare forms of aphasia, it seems reasonable to assume that the techniques you already have in place for managing Transcortical Sensory aphasia should be similar to those you use with Wernicke aphasia. Similarly, the techniques for managing Broca aphasia can be appropriate for Transcortical Motor aphasia. Do you agree with this assumption? What would be their limitations?
For Millie and Donna, is further direct individual treatment justified? If you think so, why? If not, why not? What could either one of them say to you that might convince you to pursue further treatment.
CAUTIONARY NOTE
Example #16
We end our Grand Rounds on a cautionary note with Ted, our final example. Although aphasia types are sometimes easily distinguished, as in most of the samples we have presented, other aphasias cannot be be neatly categorized. This is true even when our categories are “objective”. We have adhered to the classification outcomes from our participants’ Western Aphasia Battery test performances in this presentation. Although the WAB relies on objective measures in most instances, a critical part of classifying type of aphasia lies in making a clinical judgment on the rating scale for “Fluency” in the WAB’s Spontaneous Speech section.
Ted, our final speaker illustrates how a slightly different fluency rating (on the WAB’s Conversational Questions and Picture Description) can influence classification. Based on the WAB scoring criteria, a rating of “4” versus “5” distinguishes non-fluent from fluent aphasia types. In Ted’s case, it is hard even for experienced clinicians to agree on his score. Given his other WAB subtest scores (Auditory Comprehension, Repetition, and Naming), a Fluency rating of “5” would put him in the Anomic category and a Fluency rating of “4” would put him in the Broca category.
A computer engineer with an advanced degree, Ted suffered a stroke in his mid-40’s. His WAB AQ is 68.5. In addition to many of the characteristics of aphasia that you’ve already heard in other examples, in this segment you will hear perseveration, or the inappropriate re-use of a word that was used earlier (perhaps correctly) but is not correct in subsequent uses. This is a relatively commonly occurring feature of aphasia and other acquired neurological communication disorders. Listen to his story about the Umbrella picture sequence and consider how his fluency compares to others you’ve seen.
Umbrella

Questions for discussion
Did you notice how frequently Ted noted, “I know it but I can’t say it.”? People with aphasia often say this. Believe it; mostly it is true.
Did you note the little runs of fluency that most frequently came when Ted was “speaking for” someone else (e.g., the mom, the little boy)?
Throughout this example, Ted sought for the word “umbrella”. What techniques did he use to signal it? How effective were they? Could some of them count as perseverations? What word was his perseveration word? Did he ever actually say “umbrella”?
Ted also went through a litany of kinship words searching for “mother”. Did he ever get there?
Did you notice Ted’s circumlocution when he had trouble with a word? Did it have the useful effect of allowing him to get his message across when his word search failed? Did it ever help him produce the intended word?
And NOW … do you think he has Broca aphasia or Anomic aphasia? Why? Does this make a difference in what you would do with him in treatment?
Treatment focus -- Ted
What would your first instinct be for Ted’s treatment -- increasing his fluency, improving his word-finding skills, reducing the telegraphic nature of his output, or something else?
Could you make a case for INCREASING Ted’s circumlocutory skills? If so, what would that case be?
FINAL THOUGHTS
All of the people you have observed here are members of aphasia centers or participate in clinical activities or research programs at colleges or universities. This means that they have “voted with their feet” and have chosen to participate in programs designed to help them return to their lives as they were lived before aphasia, to seek community, and to find social connections with others who experience aphasia as well. Their willingness to be a part of AphasiaBank and to contribute their speech and language to helping others with aphasia is a strong indicator of their resilience and spirit. Regardless of the severity of their aphasia, they have indicated their willingness to educate students, provide language samples to researchers, and move the study of aphasia along in terms of both linguistic and psychosocial goals.
We thank all staff members from all the programs who have opened their doors to us. We also thank all the persons with aphasia who have contributed to our vision. Specifically, we thank individuals from the following programs who were included as examples for this project. We chose them from among literally hundreds of candidates because they so well exemplified the problems we highlighted.
Adler Aphasia Center -- Maywood NJ
Aphasia Center of California -- Oakland, CA
Aphasia Center of Tucson (ACT) -- Tucson AZ
Aphasia Center of West Texas (ACWT) -- Midland, TX
Aphasia Groups, Montclair State University -- Montclair NJ
Arizona State University Aphasia Group -- Tempe AZ
Snyder Center for Aphasic Life Enhancement (SCALE) -- Baltimore, MD
Stroke Aphasia Recovery Program (STAR)--Lubbock, TX
Stroke Comeback Center -- Vienna, VA
Triangle Aphasia Project (TAP) -- Carey, NC
University of Massachusetts Aphasia Research Program -- Amherst, MA